
In the case of vomiting animals, it is necessary to differentiate excess saliva in the mouth from mucous membrane moisture. If the membranes themselves are dry or sticky, it may indicate dehydration. This is most easily accomplished by sliding a finger along a patient’s gum line or inside the cheeks. Age is another factor to consider: loss of skin turgor progresses with increasing age, and neonates exhibit very little skin tenting even when dehydrated.Īnother way to check for dehydration is to feel for moistness on the mucous membranes. The skin tent test can be confounded by both emaciation (decreased turgor even if euhydrated) and obesity (increased turgor in the face of dehydration) and must be considered in relation to other parameters and physical examination findings. 1,5 When performing this test, veterinary technicians can often appreciate a “tacky” or “sticky” feeling in the underlying tissue, which is further evidence of dehydration. If the tent formed remains standing, it can be an indication of dehydration. In a well-hydrated animal, the skin immediately returns to its normal resting position. To perform this test, the skin over the thorax or lumbar region is pulled away from the back. One of the easiest to perform is a skin tent test to check the turgor, or moisture level, of the skin. Hydration status can be assessed using several simple tests. 5 Dehydration must not be confused with hypovolemia: dehydration describes a water deficit in the interstitial and intracellular compartments, whereas hypovolemia describes a loss of fluid in the intravascular space. Any patient determined to be more than 10% dehydrated is considered severely dehydrated 4 and requires immediate fluid resuscitation and careful monitoring. If severe, dehydration can be detected in derangements in forward perfusion parameters 1 as well as by the tests listed below. Loss of fluid from the intracellular and interstitial compartments leads to dehydration. 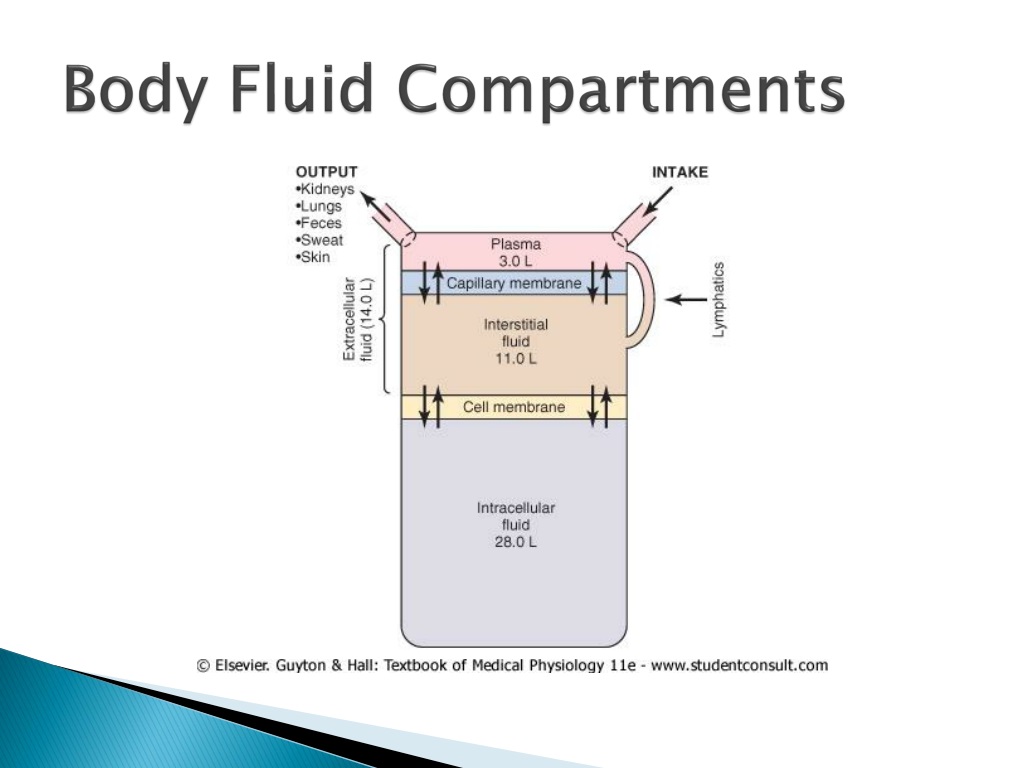
Restoring perfusion and, subsequently, oxygen and nutrient delivery to tissues is crucial to survival in these patients. If allowed to persist, this imbalance can lead to acute decompensation and death. Shock is defined as the critical imbalance between the delivery of oxygen and nutrients (carried by blood) to tissues and the tissues’ demand for these components. Patients that cannot adequately perfuse their tissues require immediate intervention with fluid therapy to restore perfusion and correct shock. The veterinary staff must assess whether the patient is perfusing its tissues well, check for dehydration, and evaluate losses from any of the fluid compartments. The first step in determining whether a patient needs fluid therapy is a full physical examination, including collection of a complete history. Veterinary professionals provide fluid therapy to patients for many reasons, including correction of dehydration, expansion and support of intravascular volume, correction of electrolyte disturbances, and encouragement of appropriate redistribution of fluids that may be in the wrong compartment (e.g., peritoneal effusion). This knowledge helps guide both fluid choice and the method used to administer fluid therapy. When providing fluid support to patients, technicians must keep in mind which compartment needs to be replenished or what derangement needs to be corrected. In addition to losses, fluid can and does move between compartments in a dynamic and ever-changing fashion. In the case of hemorrhage, for example, fluid is lost from the intravascular space (i.e., plasma) but also from the ICF in the cells lost (e.g., red blood cells, white blood cells). These differences are greatest in premature babies, when ECF exceeds ICF.The body is considered a closed system, meaning that any fluid lost must come from one of the compartments listed above. The ICF volume is obtained by subtracting the ECF volume from the TBW.ĮCF exceeds 30% and ICF is <40%. The interstitial fluid volume is determined as the difference between ECF volume and plasma volume. These substances neither leave the vascular system nor penetrate the erythrocytes. Plasma volume can be measured either by radioactive albumin or by Evans blue. ECF volume is measured using inulin, which is proportionally distributed between plasma volume and interstitial volume. TBW is measured using deuterium oxide (heavy water). Vol1 = volume of indicator, Vol2 = volume to be measured.Īgents used for measurement of fluid compartments Relationship between the volumes of major fluid compartmentsĪ known amount of tracer is introduced into the space to be measured, and its concentration measured after mixing.Ĭon1 = initial concentration of indicator, Con2 = final concentration of indicator Total body water (TBW) constitutes 55-60% of the body weight in men and 45-50% of the body weight in young women.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
